Making an Impact: COVID-19

Wagner Study Finds COVID-19 Devastates Microfinance
After surveying 1,000 microenterprise owners and 200 loan officers in Pakistan, NYU Wagner professor Jonathan Morduch and other economists have found that the financial impact of the pandemic has been devastating for poor entrepreneurial households that rely on microloans to keep small business ventures going.
In the new study in the Oxford Review of Economy Policy, Morduch and Timothy Ogden, both of Wagner’s Financial Access Initiative (FAI), along with colleagues from Oxford and Lahore, describe the highly precarious condition of microfinance customers created by the restrictions on mobility designed to limit the spread of COVID-19. In the weeks following the lockdown, borrowers’ sales and income fell by 90% and food security became their topmost immediate concern; most reported having no way to repay debt. The study offers insights for policy reform in response to the crisis.
Photo by zms / Getty Images
Setting Up a COVID-19 Testing Site
Samuel Schaffzin (MPA-HPAM 2003) is a Captain in the United States Public Health Service (USPHS) Commissioned Corps and recently returned from a deployment in support of the COVID-19 response where he helped set up a federally-supported, state-run, community-based COVID-19 testing site.
Read more about Samuel's impact

Faculty Commentary on COVID-19
Coronavirus test: What makes a good leader in times of crisis?
Professor Paul Light in Christian Science Monitor
Housing Policy Must Change in Wake of COVID-19
Professor Ingrid Gould Ellen, Professor Katherine M. O'Regan, and Sophie House (NYU Furman Center) in ShelterForce
NY has hit its COVID-19 apex, but that doesn't mean the virus is going away
Dean Sherry Glied in City & State

"I am currently working at the Department of Health and Human Services in the Substance Abuse and Mental Health Services Administration (SAMHSA). SAMHSA is awarding emergency funding to assist state health departments and tribal communities with the mental health impacts of COVID-19. Such funding is intended for communities to build their crisis support and intervention systems, offer evidence-based services (e.g., motivational interviewing, assertive community treatment, Zero Suicide, eye movement therapy, etc.) to those with substance abuse and mental health issues, and support behavioral healthcare providers who may also be impacted by their patients' suffering. I supported the review process for these grant allocations of about $2 million per entity, evaluating the strengths and weaknesses of each applicant, and made recommendations for funding determinations. It was a privilege to be involved in such efforts."
- Amanda Doreson (MPA 2011)
Social Science Analyst, Substance Abuse and Mental Health Services Administration
WAGTalks: The COVID-19 Series

How Disasters Shape NYC | Part 1
Professor Mitchell L. Moss, an expert on New York City, offers a fresh perspective on the city’s capacity to respond and recover from disasters.
US Health Policy and the COVID Pandemic
Dean Sherry Glied, a health economist, offers insights on US health policy amidst the global pandemic.
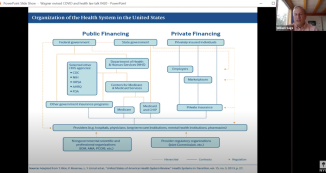
US Health Law and COVID-19
Bill Sage, Visiting Professor of Law at NYU, sheds light on US health laws in regards to coronavirus.

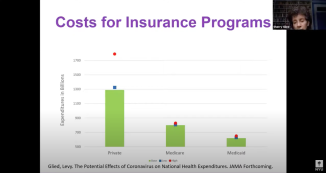
Wagner Dean Predicts America’s Health Costs as Share of GDP Will Rise
Last month, the Department of Human Services projected public and private expenditures for healthcare to grow from 17.8% to 19.7% of gross domestic product (GDP) over the next 10 years. But COVID-19’s rapid spread has scrambled such forecasts, writes NYU Wagner dean and professor of public service Sherry Glied in an article in the latest JAMA, “The Potential Effects of Coronavirus on National Health Expenditures” (Apr. 27).
Commenting with coauthor Helen Levy of the University of Michigan, Glied explains that the fractional share of US economic output represented by healthcare expenditures is likely to rise due to: 1) the surge in pandemic-related health spending (numerator) for ventilators, PPE, and other expenditures to treat patients, and 2) the previously unimagined decline in GDP (denominator) given the stalled US economy.
While health spending relative to overall US economic output is likely on the way up, “it would be better if it [health spending] were higher still: if more personal protective equipment were available if ventilators were not in short supply, and, critically, if there were more effective ways to reduce morbidity and mortality among patients with COVID-19,” Glied and Levy write.
Photo Credit: Marchmeena29 /Getty Images
"Currently, I am working at NYC Emergency Management. As a part of the activation operations of NYC Emergency Management, I have been working at the Javits NY Medical Station in the Transportation Branch to support transportation needs in the City and provide planning support to various operations at the Javits NY Medical Station. Separately, I have been working on one of our planning teams that helps adjust our internal emergency response plans to ensure they take into consideration the impacts of COVID-19 (i.e. social distancing, remote work, school closures, etc.)."
- Staphany Lu (MPA 2018)
Transportation and Infrastructure Planner, New York City Emergency Management Department


The Cordon Sanitaire Returns Amid Global Contagion
In response to the spread of COVID-19, the Qatari government has sealed off a 12-square-kilometer zone that houses migrant laborers working on large projects for the 2022 World Cup. But as opposed to blunting the contagion, the area’s densely populated dormitories, with limited ventilation and poor sanitation, favor the novel coronavirus's swift spread, according to Natasha Iskander, a migration scholar at NYU Wagner. And the laborers from South Asia, the Middle East, and Africa are permitted to leave the residential area only aboard buses taking them to construction sites where they work “elbow to elbow,” sharing tools.
Writing in Items, a digital forum of the Social Science Research Council, Iskander explains that cordons sanitaires are not new: they have been used in many countries during the past century or more – for example, during an 1892 typhus scare in New York’s Russian Jewish-suffused Lower East Side. But as contagious diseases are not easily deterred by barricades or roadblocks, these kinds of social and spatial divides have been primarily intended to further another objective – “as a boundary that maps out zones of political exclusion rather than as a means of disease control.”
Share Your Story and Efforts on COVID-19
Are you a member of the NYU Wagner Community? Your story matters in this extraordinary moment.
READY TO MAKE YOUR IMPACT?
Learn how an NYU Wagner education can get you there.
